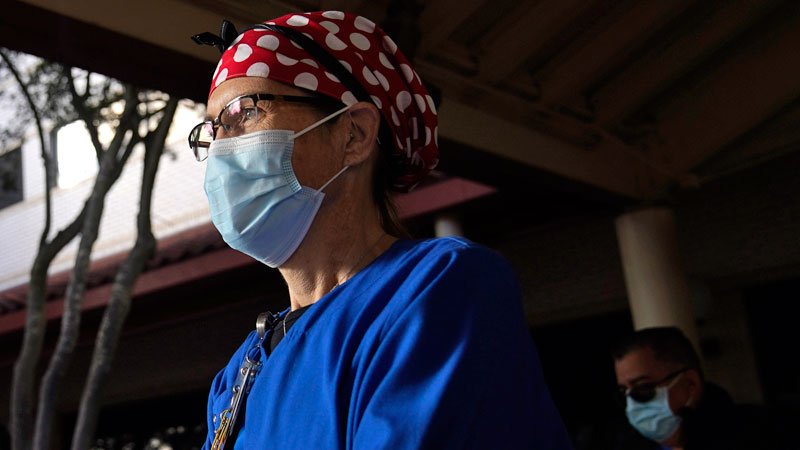
For Nurses Feeling the Rigidity of the Pandemic, Virus Resurgence Is ‘Paralyzing’
Editor’s demonstrate: Get the most contemporary COVID-19 news and guidance in Medscape’s Coronavirus Resource Heart.
For Christina Nester, the pandemic lull in Massachusetts lasted about three months through summer season into early fall. In late June, St. Vincent Sanatorium had resumed optionally accessible surgeries, and the unit the 48-365 days-used nurse works on switched support from taking care of handiest COVID-19 patients to its pre-pandemic roster of patients improving from gallbladder operations, mastectomies and other surgeries.
That is, unless October, when patients with coronavirus infections began to reappear on the unit and, with them, the fear of many extra to advance. “It is paralyzing, I’m now not going to lie,” acknowledged Nester, who’s labored on the Worcester scientific institution for just about 2 a long time. “My tiny clan of nurses that I work with, we worried when it began to uptick here.”
Along side to that stress is that nurses are caught betwixt caring for the bedside desires of their patients and implementing policies build by others, reminiscent of doctor-ordered treatment plans and strict scientific institution principles to assign off the coronavirus. The push-pull of those forces, amid a fight against a virus, is straining this crucial spine of successfully being suppliers nationwide, and that can additionally accumulate to unstainable ranges if the virus’s surge is now not contained this winter, advocates and researchers warn.
Nurses utilize the most sustained time with a affected person of any clinician, and as of late patients are on the total extremely panicked and isolated, acknowledged Cynda Rushton, a registered nurse and bioethicist at Johns Hopkins College in Baltimore.
“They’ve change into, in many ways, a extra or less emotional surrogate for household participants who can’t be there, to toughen and notify and offer a human touch,” Rushton acknowledged. “They’ve witnessed unbelievable amounts of suffering and death. That, I beget, additionally weighs with out a doubt heavily on nurses.”
A look printed this autumn within the journal Traditional Sanatorium Psychiatry came all the perfect intention through that 64% of clinicians working as nurses, nurse practitioners or doctor assistants at a Fresh York City scientific institution screened positively for acute disaster, 53% for depressive symptoms and 40% for alarm — all better charges than came all the perfect intention through among physicians screened.
Researchers are fervent that nurses working in a fleet changing crisis love the pandemic — with concerns starting from workers shortages that curtail their time with patients to enforcing visitation policies that upset families — can accumulate a psychological response known as “factual demolish.” That demolish occurs, they are saying, when nurses with out a doubt feel stymied by their incapability to present the stage of care they think patients require.
Dr. Wendy Dean, co-founder of Like minded Damage of Healthcare, a nonprofit organization based in Carlisle, Pennsylvania, acknowledged, “Doubtlessly the final discover driver of burnout is unrecognized unattended factual demolish.”
In parts of the nation over the summer season, nurses got some psychological successfully being respite when cases declined, Dean acknowledged.
“No longer enough to with out a doubt route of it all,” she acknowledged. “I beget that is a route of that can intention shut quite lots of years. And it be doubtlessly going to be extended for the reason that pandemic itself is extended.”
Sense of Powerlessness
Before the pandemic hit her Massachusetts scientific institution “love a woodland fire” in March, Nester had infrequently ever viewed a affected person die, as a replace of any individual within the final discover days of a illness love cancer.
All of sudden she modified into fervent with frequent transfers of patients to the intensive care unit after they couldn’t breathe. She recounts tales, imprinted on her memory: The girl in her 80s who didn’t even seem unwell on the day she modified into hospitalized, who Nester helped transport to the morgue now not up to per week later. The husband and wife who beget been unwell within the intensive care unit, whereas the adult daughter fought the virus on Nester’s unit.
“Then every folk died, and the daughter died,” Nester acknowledged. “There’s now not with out a doubt words for it.”
Reliable through these gut-wrenching shifts, nurses can infrequently change into separated from their emotional toughen method — one one more, acknowledged Rushton, who has written a e-book about battling factual demolish among successfully being care suppliers. To better take care of the influx, some nurses who in general work in noncritical care areas beget been moved to love critically unwell patients. That forces them to now not handiest adjust to a novel variety of nursing, but additionally disrupts an on the total-successfully-honed working rhythm and camaraderie with their traditional nursing co-workers, she acknowledged.
At St. Vincent Sanatorium, the nurses on Nester’s unit beget been urged one March day that the primarily postsurgical unit modified into being transformed to a COVID unit. Nester tried to squelch fears for her be pleased security whereas comforting her COVID-19 patients, who beget been on the total aged, terrified and infrequently now not easy of hearing, making it now not easy to focus on through layers of masks.
“You may well very successfully be attempting to deliver through all of these boundaries and strive to level to them in conjunction with your eyes that you are here and also you are now not going to head away them and will intention shut care of them,” she acknowledged. “But but you are panicking within entirely that it’s likely you’ll well accumulate this illness and also you are going to be the one within the bed or a household member that you love, intention shut it home to them.”
When requested if scientific institution leaders had viewed indicators of strain among the nursing workers or beget been fervent with their resilience headed into the winter months, a St. Vincent spokesperson wrote in a short assertion that for the interval of the pandemic “we beget prioritized the protection and successfully-being of our workers, and we remain obsessed with that.”
Nationally, the viral risk to clinicians has been successfully documented. From March 1 through Would possibly maybe well well honest 31, 6% of adults hospitalized beget been successfully being care workers, one-third of them in nursing-connected occupations, in accordance with files printed ultimate month by the Centers for Illness Control and Prevention.
As cases mount within the winter months, factual demolish researcher Dean acknowledged, “nurses are going to enact the calculation and dispute, ‘This risk is never value it.'”
Juliano Innocenti, a traveling nurse working within the San Francisco space, decided to intention shut off for a few months and will level of interest on wrapping up his nurse practitioner level as a replace. Since April, he’s been seeing a therapist “to navigate my powerlessness in all of this.”
Innocenti, 41, has now not been on the entrance traces in a scientific institution battling COVID-19, but he aloof feels the stress because he has been treating the public at an outpatient dialysis clinic and a psychiatric scientific institution and viewed administrative concerns generated by the crisis. He pointed to concerns reminiscent of inadequate non-public protective equipment.
Innocenti acknowledged he modified into fervent with “the inability of planning and stunning blatant brush aside for the foremost security of patients and workers.” Revenue motives too on the total force choices, he urged. “That’s what I’m taking a demolish from.”
Constructing Resiliency
As cases surge once more, scientific institution leaders must negate bigger than employee assistance programs to backstop their already depleted ranks of nurses, Dean acknowledged. Along with heaps of protective equipment, that includes helping them with every thing from groceries to transportation, she acknowledged. Overstaff a bit of, she urged, so nurses can intention shut a demolish day after they hit an emotional cliff.
The American Nurses Association, the American Association of Critical-Care Nurses (AACN) and quite lots of different nursing teams beget compiled online sources with links to psychological successfully being programs as successfully as guidelines for getting through every pandemic workday.
Kiersten Henry, an AACN board member and nurse practitioner within the intensive care unit at MedStar Montgomery Medical Heart in Olney, Maryland, acknowledged that the nurses and other clinicians there beget began to amass for a short huddle on the head of now not easy shifts. Along with talking about what took build, they portion quite lots of honest correct issues that additionally happened that day.
“It would not imply that you are now not taking it home with you,” Henry acknowledged, “but you are if truth be told verbally processing it to your visitors.”
When cases reached their highest level of the spring in Massachusetts, Nester acknowledged there beget been some days she didn’t ought to advance.
“But you know that your visitors are there,” she acknowledged. “And the most handy ones that with out a doubt truly perceive what’s occurring are your co-workers. How are you able to allow them?”